Many patients visit our clinic feeling incredibly frustrated by persistent, uncomfortable abdominal distension, also known as bloating. Sometimes, the presumed culprit is Small Intestinal Bacterial Overgrowth (SIBO) or a severe microbiome imbalance. If you’ve experienced these symptoms, you might have even taken multiple breath tests, tried restrictive diets, or taken rounds of antibiotics, only to find the uncomfortable swelling returning day after day.
The increasing use of breath testing in modern clinics has significantly narrowed the conversation around functional bloating causes. And while bacterial overgrowth is certainly a valid concern, it’s not the only explanation. In fact, many people experience severe bloating without SIBO.
At hol+ we take a deeper look at gut health, and know that digestion is not just about what is sitting in your gut, but how efficiently those contents move through it. Motility reflects the deep coordination between your nervous system, your muscles, and your metabolic state.
Explore our approach to functional digestive health>>
What Is Gut Motility?
To understand what causes bloating (if not SIBO), we first need to understand how the body naturally moves food. In systems-based medicine, digestion is not a passive event. It is an actively regulated process dependent on coordinated signaling.
Motility, Defined
Gut motility refers to the coordinated muscular contractions that move food through the gastrointestinal tract. This complex mechanical process includes stomach emptying, small intestine transit, and the final movements of the colon. When these muscular waves operate smoothly, you absorb nutrients efficiently and eliminate waste without discomfort. When they slow down, you begin to experience intestinal motility dysfunction.
The Migrating Motor Complex (MMC)
One of the most important aspects of gut health and motility is the Migrating Motor Complex, or MMC (1). Think of the MMC as your digestive system’s internal street sweeper. These cyclical “cleansing waves” occur between meals, specifically during fasting states. The migrating motor complex MMC clears residual food, debris, and bacteria from the small intestine, pushing it downward. If you are constantly eating or snacking, this cleansing wave is paused.
Nervous System Control
Your digestive muscles do not act on their own. They rely heavily on the enteric nervous system and the vagus nerve (2). This connection is heavily influenced by your autonomic nervous system. Proper digestion requires a parasympathetic state, commonly known as “rest and digest.” If your body is stuck in a stressed, sympathetic state, the signals to your gut slow down (3).
Bloating Without SIBO: What’s Actually Happening
If bacteria are not the primary culprits, then what is creating that uncomfortable pressure in your abdomen? Understanding the mechanics of slow gut motility bloating can help you find lasting relief. Bloating can definitely be a motility problem long before it becomes a microbiome problem.
Impaired Transit Time
When you have slow motility, food and gas remain in the digestive tract longer than intended. As food sits in a warm environment, it naturally begins to ferment. This fermentation produces gas, even if you do not have an abnormal overgrowth of bacteria. The longer transit time directly leads to physical distension.
Gas Handling vs Gas Production
Interestingly, some patients produce completely normal volumes of gas. The symptoms arise not from excessive production, but from impaired clearance and heightened sensitivity. If the gas cannot move efficiently through the intestines, it gets trapped. This trapping is a hallmark of digestive motility disorder symptoms.
Read: 5 Signs SIBO Is the Cause of IBS
Pressure and Distension
Slower movement naturally leads to the accumulation of both food matter and gas. This accumulation creates visible bloating and uncomfortable pressure. For many individuals experiencing slow gut motility, this distension often worsens later in the day as meals compound upon one another.
Related: IBS vs. SIBO
Why Motility Breaks Down
In root cause medicine, we go beyond symptom identification to understand how and why multiple systems contribute. Here are the primary reasons why your motility might be compromised.
1. Nervous System Dysregulation
Your gut is profoundly responsive to your nervous system. Chronic sympathetic dominance – being stuck in “fight or flight” – causes reduced vagal tone and impaired signaling to your digestive muscles (4). Constant survival signaling halts the smooth, coordinated movements of your gut.
2. Stress and the Gut-Brain Axis
Stress and metabolism directly influence digestion. The gut brain connection is powerful. Psychological and physical stress actively slows gastric emptying and intestinal transit. It disrupts MMC activity and alters how sensitive your gut feels to normal amounts of gas. In other words, a moderate amount of gas can feel extra painful.
3. Hormonal and Metabolic Influences
Your endocrine system plays a massive role in motility. Thyroid function heavily impacts how quickly your gut moves (5). Furthermore, blood sugar instability affects the energy availability required for digestive muscle contractions. Cortisol dysregulation, often stemming from chronic stress, alters your natural gut rhythm (6).
4. Post-Infectious Changes
Sometimes, intestinal motility dysfunction begins after a severe bout of food poisoning or a gastrointestinal infection (7). Even after the infection clears, damage to the delicate signaling pathways and nerves in the gut can persist. This post-infectious change is frequently mislabeled as chronic SIBO when it is actually a motility issue.
5. Dietary Patterns That Disrupt Motility
Our modern eating habits often work against our natural digestive rhythms. Constant grazing throughout the day prevents the fasting windows required for the MMC to activate. On the other end of the spectrum, very low caloric intake or highly restrictive diets can deprive the digestive tract of the energy and bulk it needs to stimulate movement (8).
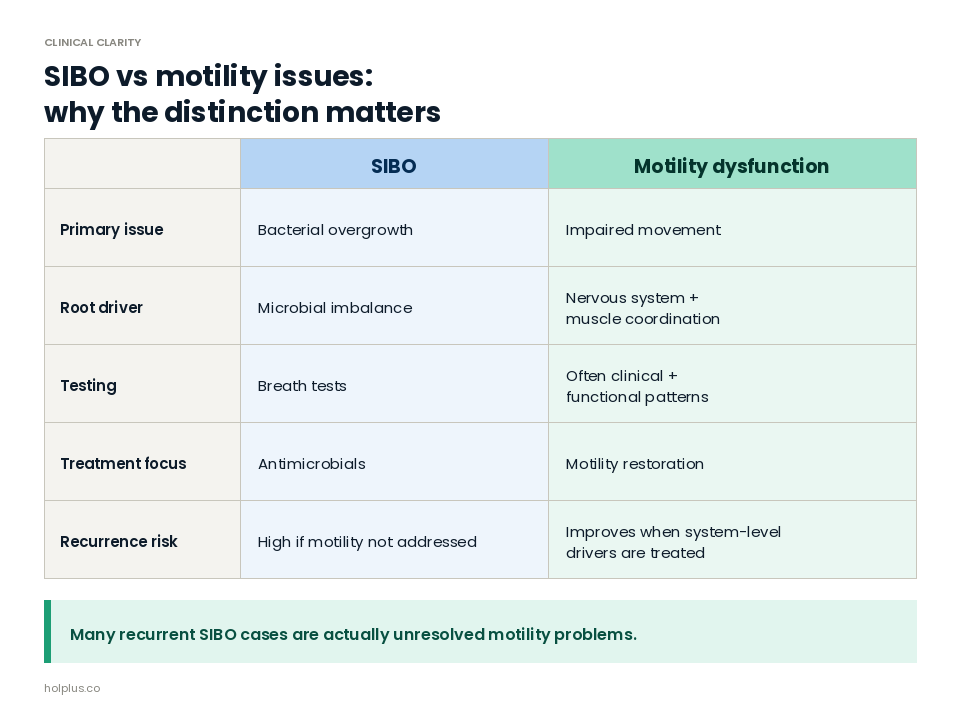
Signs Motility May Be the Root Cause of Bloating
When distinguishing between typical IBS vs motility disorder, patterns matter more than isolated symptoms. You might be dealing with a motility issue if you notice the following signs (9):
- Bloating that progressively worsens throughout the day
- Significant relief of abdominal pressure after a bowel movement
- A strong constipation and bloating connection, or a feeling of incomplete evacuation
- A persistent feeling of “slow digestion” or heaviness after eating
- Experiencing severe bloating despite eating a whole-foods diet
- Symptoms returning quickly after completing SIBO treatments
- Extreme sensitivity to large meals or frequent snacking
The Systems-Based Ripple Effect of Impaired Motility
Motility sits at the intersection of multiple bodily systems. When movement slows down, the effects ripple outward, impacting your whole-person health.
Gut Health
When food remains stagnant, increased fermentation occurs. Over time, this stagnation can create a microbial imbalance. While you may have started with bloating without SIBO, chronic slow motility can eventually create the perfect environment for secondary SIBO to develop (10).
Metabolic Health
Impaired digestion affects how you process and absorb nutrients. This can lead to blood sugar instability and significant energy fluctuations throughout the day. When your transit time is compromised, your body cannot efficiently extract the fuel it needs.
Hormone Health
Your gut is responsible for clearing metabolized hormones from your body. For example, estrogen clearance via the gut may be negatively affected by slow motility, leading to hormonal imbalances. Additionally, thyroid function both influences and is influenced by your gut motility.
Nervous System Feedback Loop
Digestive discomfort actively increases stress signaling to the brain (11). This creates a challenging feedback loop: stress impairs motility, which causes bloating and discomfort, which in turn causes more stress. Healing requires shifting away from this static noise and moving toward clear, calming signals.
Want to learn more? Schedule a FREE 15 minute consultation
Schedule Your Consultation
The Root Cause Medicine Approach to Bloating
At hol+, our root cause bloating evaluation is designed to map out your unique health landscape. Testing is used to understand system behavior, not simply to isolate a single symptom or culprit.
Structured Evaluation
Our integrative approach begins with a detailed symptom timeline. We listen carefully to your history, analyzing your meal patterns, timing, and bowel habits. We also deeply assess your stress physiology and lifestyle factors to understand how your environment interacts with your biology.
Advanced Diagnostics
When indicated, we utilize advanced diagnostics to uncover hidden barriers. This may include a comprehensive thyroid panel, metabolic markers, and inflammatory markers. We also use targeted gut health testing to see the full picture of your microbiome and digestive function, ensuring we address both the structural and biochemical aspects of your health.
Related: Metabolic Markers for Digestive Health
Restoring Motility: A Systems-Based Strategy
Resolving functional medicine bloating requires a comprehensive, personalized plan. We blend the best of clinical science and holistic traditions to restore your body’s natural rhythm.
Nervous System Regulation
Because nervous system digestion is so tightly linked, regulating your nervous system is a priority. We can guide you through targeted breathwork and vagal stimulation techniques. By prioritizing sleep optimization and reducing chronic sympathetic (fight or flight) activation, we help your body return to a state of safety and repair.
Meal Timing and Digestive Rhythm
We support your migrating motor complex by optimizing your meal timing. This often involves spacing meals appropriately to allow the MMC to sweep the intestines clean. By avoiding constant grazing and aligning your eating patterns with your natural physiology, we encourage healthy digestive transit.
Metabolic Stabilization
A balanced macronutrient intake is crucial for consistent energy. We work with you to ensure blood sugar regulation and adequate caloric intake, giving your digestive muscles the fuel they need to contract smoothly and efficiently.
Targeted Support
When clinically appropriate, we utilize targeted support to jumpstart your motility. This may include natural prokinetic strategies, nutrient repletion, and specific herbal or pharmaceutical support. We blend ancient botanical wisdom with cutting-edge medical expertise to gently encourage movement.
Movement and Lifestyle
Physical movement encourages digestive movement (12). We integrate light physical activity, such as walking after meals, to naturally support transit time. Paired with stress resilience practices, this creates a supportive environment for complete system-level health.
Get to the Root Cause of Bloating
Persistent bloating is not always a bacterial issue. Motility is a foundational, yet frequently overlooked driver of abdominal discomfort. Addressing your root causes requires looking far beyond the microbiome and honoring the intricate connections within your body.
At hol+, your bloating is evaluated within the broader human health operating system. We are dedicated to ensuring that your gut function is restored through coordinated, system-level care rather than temporary symptom suppression alone. We are here to support your journey, bringing balance back to your body, and peace of mind to your daily life.


